Melanoma
Understanding and Preventing Melanoma: A Life-Threatening Skin Cancer
Melanoma is a serious form of skin cancer that originates in melanocytes, the cells responsible for producing melanin, the pigment that gives skin its color. While melanocytes are predominantly located in the skin, they can also be found in the eyes, bowel, and other parts of the body. However, the risk of developing melanoma outside the skin is much lower.
Although melanoma is less common than other skin cancers, it is the most lethal, accounting for roughly 75% of all skin cancer-related deaths. In the U.S., approximately 160,000 new cases of melanoma are diagnosed each year. Excessive exposure to ultraviolet (UV) light is a significant risk factor for developing melanoma.
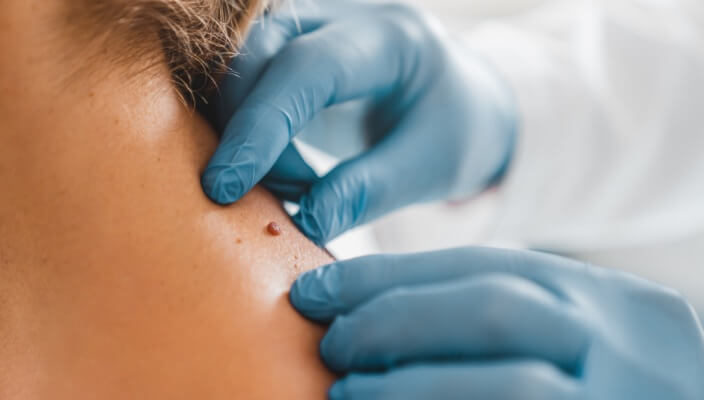
Regular skin checks by a dermatologist are essential for detecting melanoma, which can be life-threatening if not caught early. Dermatologists are trained to identify suspicious moles, lesions, or skin changes that may indicate melanoma. In addition to professional evaluations, self-examinations are equally important. Monitoring moles for changes in shape, size, color, or the emergence of new spots can help in the early detection of melanoma.
Combining professional dermatological assessments with self-exams enhances the likelihood of early detection, which is critical for successful treatment and improved outcomes. Regular skin checks and self-examinations are vital for maintaining overall skin health and catching melanoma in its earliest, most treatable stages.
Learn more about Melanoma and the treatment options available at Cumberland Skin below. Schedule an appointment with us today.
Examples of Melanoma
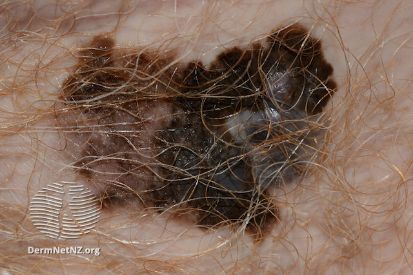
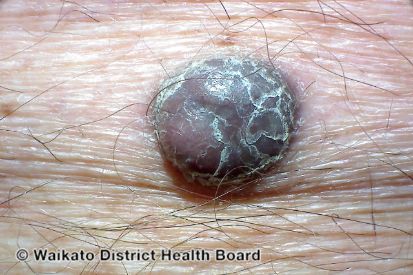

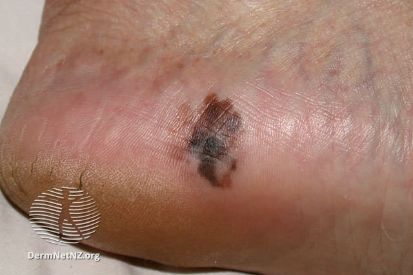
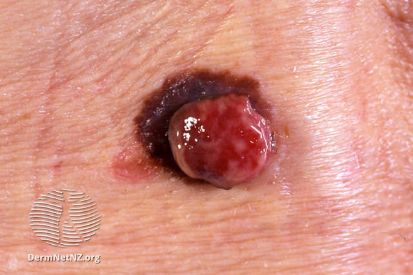
Symptoms of Melanoma
- Melanoma most often presents itself with the change of an existing mole, including change of symmetry, color, or shape.
- Irregular mole borders – scalloped, wavy, or notched.
- Diameter - anything new growing in size.
- Moles that itch, ooze or bleed.
- Melanoma can appear on normal skin tissue and does not always start as a mole.
What Causes Melanoma?
- Melanoma is primarily caused by the uncontrolled growth of pigment-producing cells (melanocytes) in the skin.
- Melanoma is often triggered by exposure to ultraviolet (UV) radiation from sunlight or tanning beds.
- Genetic factors and a history of severe sunburns also contribute to the development of melanoma.
How to Prevent Melanoma
Melanoma FAQs
The main cause of melanoma is exposure to ultraviolet (UV) radiation from sunlight or tanning beds. Other risk factors include fair skin, a history of sunburns, having numerous moles, a family history of melanoma, and a weakened immune system.
Diagnosis involves a biopsy, where a sample of the suspicious area is removed and examined under a microscope. Dermatologists may use the ABCDE rule (Asymmetry, Border irregularity, Color variations, Diameter larger than 6mm, Evolution or change) to assess whether a mole may be melanoma.
Melanoma is staged from 0 to IV, with stage 0 being melanoma in situ (confined to the top layer of skin) and stage IV indicating that the cancer has spread to other organs. Staging helps determine the extent of the disease and guides treatment decisions.
Treatment options for melanoma depend on the stage of the cancer and may include surgical excision, lymph node removal, immunotherapy, targeted therapy, radiation therapy, or chemotherapy. The choice of treatment is individualized based on factors such as the patient's overall health and the characteristics of the melanoma.
A skin check, or Total Body Skin Exam, performed by a dermatologist involves a thorough examination of the skin to identify any abnormalities, including moles, lesions, or other signs of skin conditions or skin cancer. This examination may be part of a routine check-up or may be prompted by specific concerns. The dermatologist assesses the size, shape, color, and texture of moles, and may perform additional tests or biopsies if necessary for further evaluation. Regular skin checks are essential for early detection and management.
You should apply sunscreen every day, regardless of weather. Even on cloudy days and during the winter, UV rays can still penetrate the clouds and cause skin damage. Sunscreen needs time to be absorbed into the skin. Apply it at least 15-30 minutes before going outdoors and reapply every two hours.
From Our QualDerm Family of Brands: Melanoma Treatment Options
Melanoma Treatment Options
We will confirm melanoma through a biopsy and pathological examination and then treat appropriately.
Treatment options for melanoma provided by a dermatologist may include surgical procedures to remove the cancerous tissue, such as excision or Mohs surgery. Additionally, your dermatologist may recommend therapies like immunotherapy, targeted therapy, or chemotherapy, depending on the stage and characteristics of the melanoma. Close monitoring, regular skin checks, and collaboration with other specialists ensure effective treatment and reduce the risk of recurrence.
If you notice unusual growths on your skin as mentioned above, we highly recommend scheduling an appointment with one of our providers. Annual skin checks are essential for early detection.
Early detection and treatment are crucial elements of comprehensive skin cancer care.
Related Blog Posts
- Skin Cancer
- Skin Exams
With skin cancer cases rising year after year, it’s no surprise that people are itching to learn more about this life-threatening skin disease
Read More
- Skin Cancer
- Skin Exams
It’s time to face the facts: skin cancer can develop in individuals of all skin colors, including those with darker skin tones.
Read More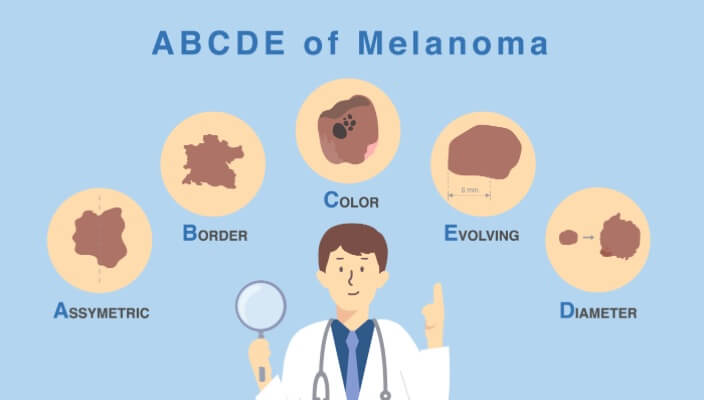
- Skin Cancer
- Skin Exams
Discover the ABCDEs of melanoma. Familiarize yourself with the five key indicators to aid in early detection and prompt medical attention for any suspicious moles or skin lesions.
Read MoreFeatured Products for Sun Protection

EltaMD UV Clear SPF 46 original
Oil-free EltaMD UV Clear helps calm and protect sensitive skin types prone to discoloration and breakouts associated to acne and rosacea. It contains niacinamide (vitamin B3), hyaluronic acid and lactic acid, ingredients that promote the appearance of healthy-looking skin. Very lightweight and silky, it may be worn with makeup or alone. Choose from tinted and untinted formulas for use every day. 1.7 oz / 48 g

EltaMD UV Sport SPF 50 3oz, 7 oz
Have your fun in the sun – but play it safe. This sunscreen is great for swimmers, skiers, runners, golfers and other athletes – or for those who just love to be outdoors! UV Sport is water-resistant, so it won’t rinse off in water or drip into your eyes and sting when you sweat.


